SHOULDER PAIN · PILLAR GUIDE · LOGANSPORT, IN
Shoulder Pain in Logansport, IN: 7 Common Causes (and What Helps)
Most shoulder pain follows a pattern. Match the plan to the pattern—don’t guess.
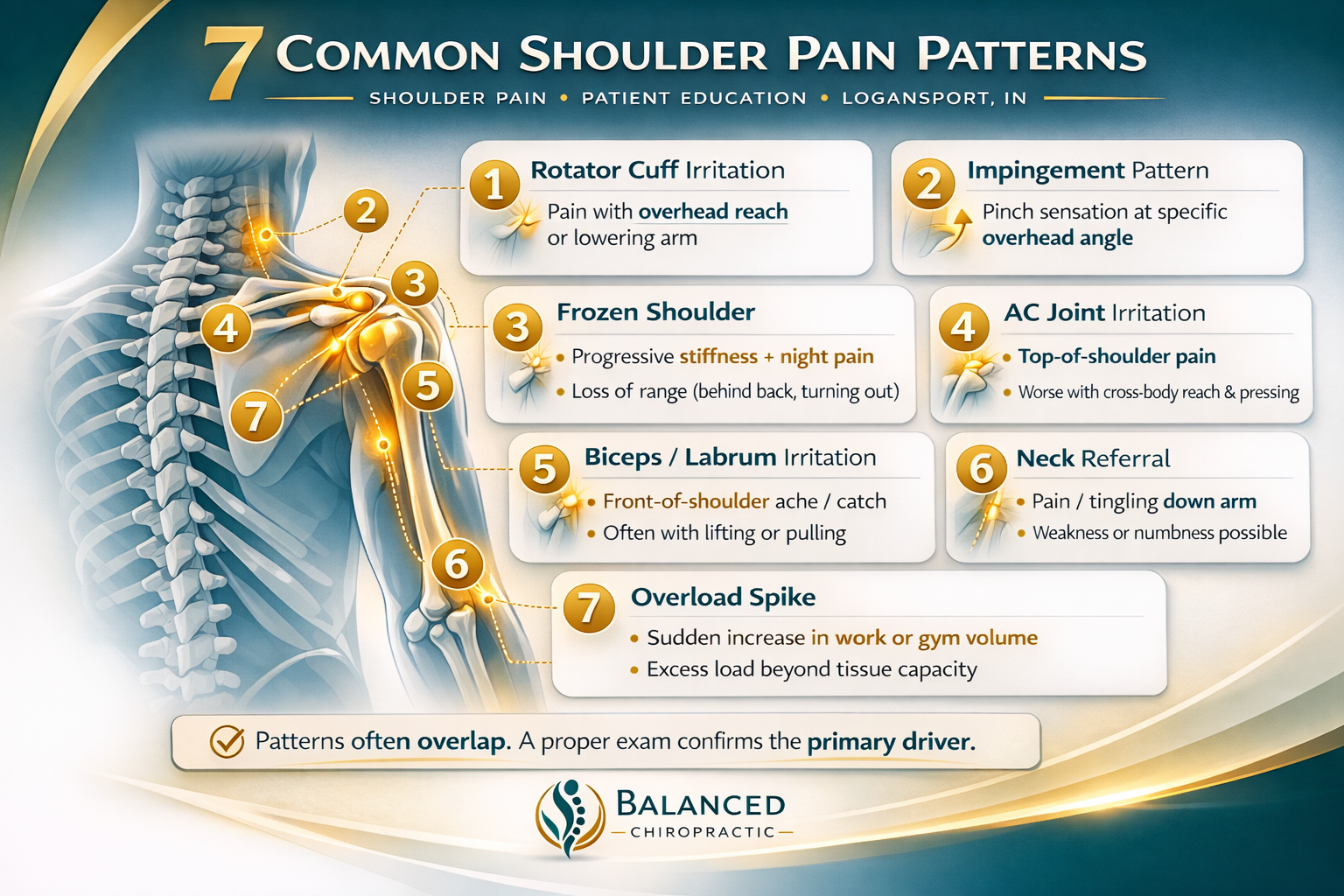
Shoulder pain can make sleeping, lifting, reaching, and work feel impossible. The fastest way forward is identifying the likely driver and choosing a plan that restores motion and strength safely. If symptoms persist or keep returning, start with Shoulder Pain Treatment. For comparison-style sorting, see Rotator Cuff vs. Impingement vs. Frozen Shoulder.
- We assess shoulder + scapula + neck together
- Conservative plan: calm irritation, restore motion, rebuild strength
- Clear “when to worry” red flags included below
Educational only. Not medical advice. Seek urgent care for severe/worsening symptoms or red flags.
Start Here: “Big Clues” That Narrow Shoulder Pain Fast
Not a diagnosis—just a smarter way to decide which direction to read first.
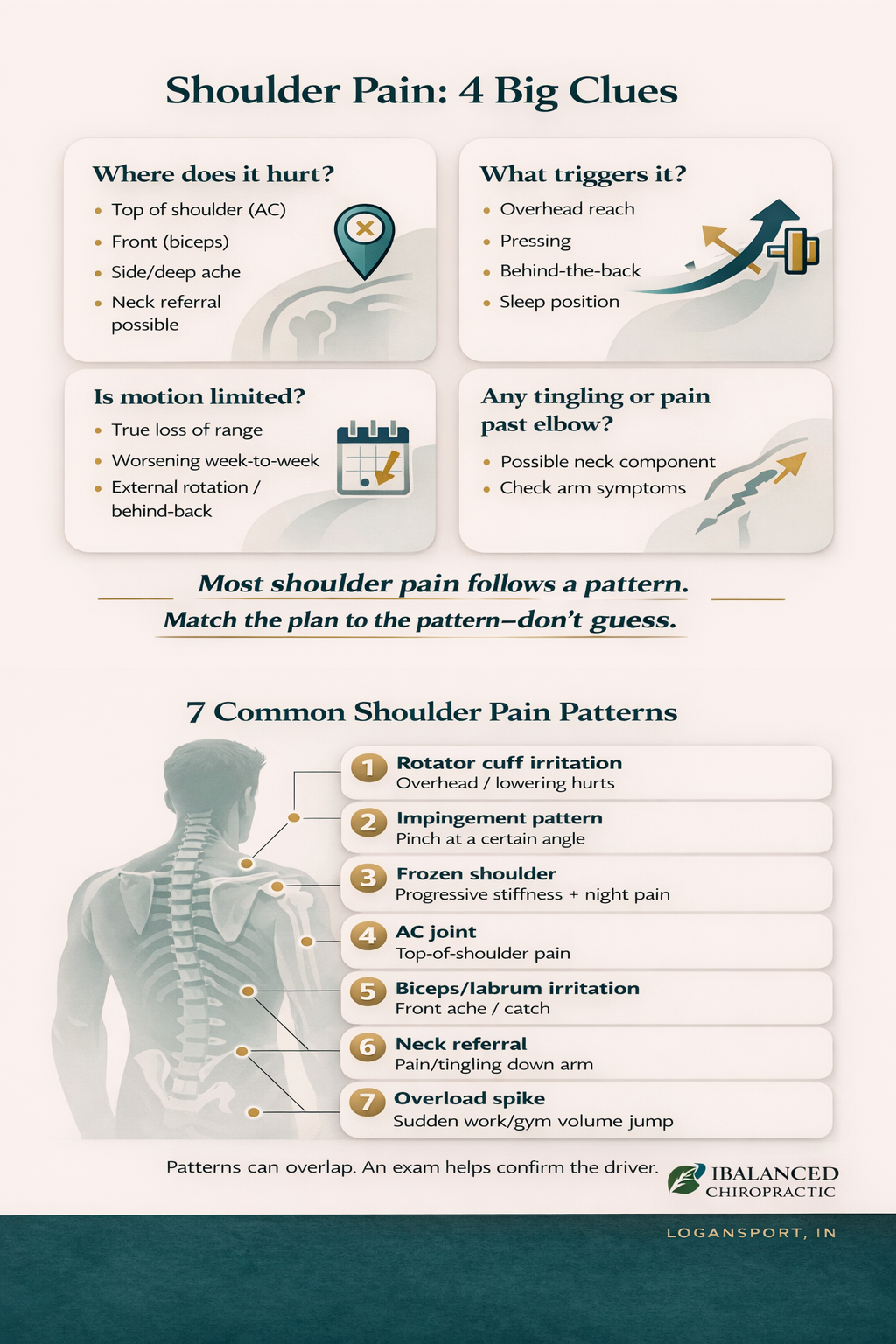
1) Where does it hurt most?
Top of shoulder (AC joint area), front of shoulder (biceps area), side/deltoid area, deep ache, or pain traveling down the arm can point to different buckets.
2) What triggers it most?
Overhead reach, pressing, reaching behind your back, sleeping on the side, or repetitive lifting at work/gym all suggest different drivers.
3) Is motion truly limited (blocked), or just painful?
True loss of range that worsens week-to-week follows a different pathway than soreness after a workload spike.
4) Any tingling, numbness, or symptoms past the elbow?
If yes, a neck component is more likely. Read: Neck Pain with Arm Tingling.
Common Shoulder Pain Patterns (and What Usually Helps)
Each pattern gets a different “first step.” Don’t force the wrong plan.
Pattern 1) Rotator cuff irritation (tendon overload)
Often feels like: pain lifting away from the body or lowering the arm from overhead.
- Usually helps: short-term load reduction + progressive strengthening
- Fast win: reduce overhead volume 7–14 days; add pulling volume
- Read next: Lifting Shoulder Pain Mistakes & Fixes
Pattern 2) Impingement-type pain (often mechanics + load)
Often feels like: “pinch” at a certain angle, especially overhead.
- Usually helps: scapular control + thoracic mobility + graded strength
- Fast win: neutral grip pressing and pain-safe ranges
Pattern 3) Frozen shoulder (stiff + blocked)
Often feels like: true stiffness with progressive loss of motion (especially external rotation and behind-the-back reach).
- Usually helps: staged mobility (not aggressive stretching) + a consistent plan
- Fast win: stop forcing sharp stretches; use low-intensity daily mobility
- Read next: How to Tell Which One It Is
Pattern 4) AC joint irritation (top-of-shoulder pain)
Often feels like: pain right at the top of the shoulder near the collarbone, worse with cross-body reach and pressing.
- Usually helps: modify pressing angles and reduce heavy deep pressing briefly
- Fast win: avoid dips/deep bench volume for 2–3 weeks
Pattern 5) Neck referral masquerading as shoulder pain
Often feels like: symptoms down the arm or past the elbow; tingling/numbness; “nerve-y” behavior.
- Usually helps: treat the driver (neck + scapula mechanics), not just the shoulder
- Read next: Neck Pain Causes & Red Flags
What Helps Most (A Simple 3-Step Plan Ladder)
Use this structure to reduce guesswork and prevent re-irritation.
Step 1: Calm the flare (first 7–10 days)
- Reduce the one movement that reliably spikes symptoms (often overhead, deep pressing, or side-sleep compression)
- Keep pain-safe motion daily
- Stop “testing” painful ranges multiple times per day
Step 2: Restore motion + rebuild strength (weeks 2–6)
- Progress range first, then strength
- Bias pulling/upper back volume for many shoulder patterns
- Gradually reintroduce overhead work only when tolerance improves
Step 3: If it’s not improving
- Get an exam to confirm the primary driver (shoulder + scapula + neck)
- If you’re losing motion week-to-week, treat it as a stiffness pathway
- Consider imaging when red flags are present or progress stalls despite a smart plan
When to Worry (Red Flags)
Get checked promptly if any of these are true.
- Sudden weakness after an injury (can’t lift the arm like before)
- Visible deformity, major swelling/bruising, suspected fracture/dislocation
- Rapidly worsening pain or escalating night pain
- Numbness/tingling with weakness down the arm
- Fever with a hot/red swollen shoulder
- True loss of motion that worsens week-to-week
Not sure? Start with Contact & Location and we’ll guide you.
Shoulder Pain FAQs
Quick answers—including “when to worry.”
Leave a Reply