KNEE PAIN · STAIRS SELF-SORTER · LOGANSPORT, IN
Knee Pain on Stairs: Why It Happens (and 5 Fixes That Usually Help)
Stairs load the knee harder than flat walking—so small issues show up fast. Use the self-sorter and the 5-fix plan.

Knee pain on stairs is common in Logansport—especially if your workload or activity volume recently increased. If you want the full knee overview, start here: Knee Pain Treatment. If you’re trying to self-sort meniscus vs runner’s knee patterns, see Runner’s Knee vs. Meniscus.
- 60-second self-check + pattern map
- 5 fixes with dosing (what to do first)
- Clear “when to worry” guidance
Educational only. Not medical advice. Patterns overlap—an exam confirms the driver.
Quick Answer (Why Stairs Hurt)
Stairs increase knee bend (knee flexion) and joint/tendon load. That means small irritations can flare quickly—especially if quad/hip capacity isn’t keeping up.

Most common drivers
- Patellofemoral load (front-of-knee / kneecap pattern)
- Tendon overload (patellar tendon)
- Capacity gap (quads/hips/endurance not matching stair volume)
What usually works first
- Reduce the spike (volume/step height/pace) for 7–14 days
- Rebuild quads + hips with pain-safe progression
- Technique tweaks (downstairs especially)
60-Second Self-Check (Pattern Sorter)
Answer quickly. The goal is direction—not certainty.
How to interpret it
- Front pain + down worse: often patellofemoral / quad capacity pattern.
- Front pain below kneecap: often patellar tendon overload.
- Inside joint line + swelling/catching: meniscus/arthritis patterns → get checked if persistent.
- Swelling/locking/giving way: evaluate sooner.
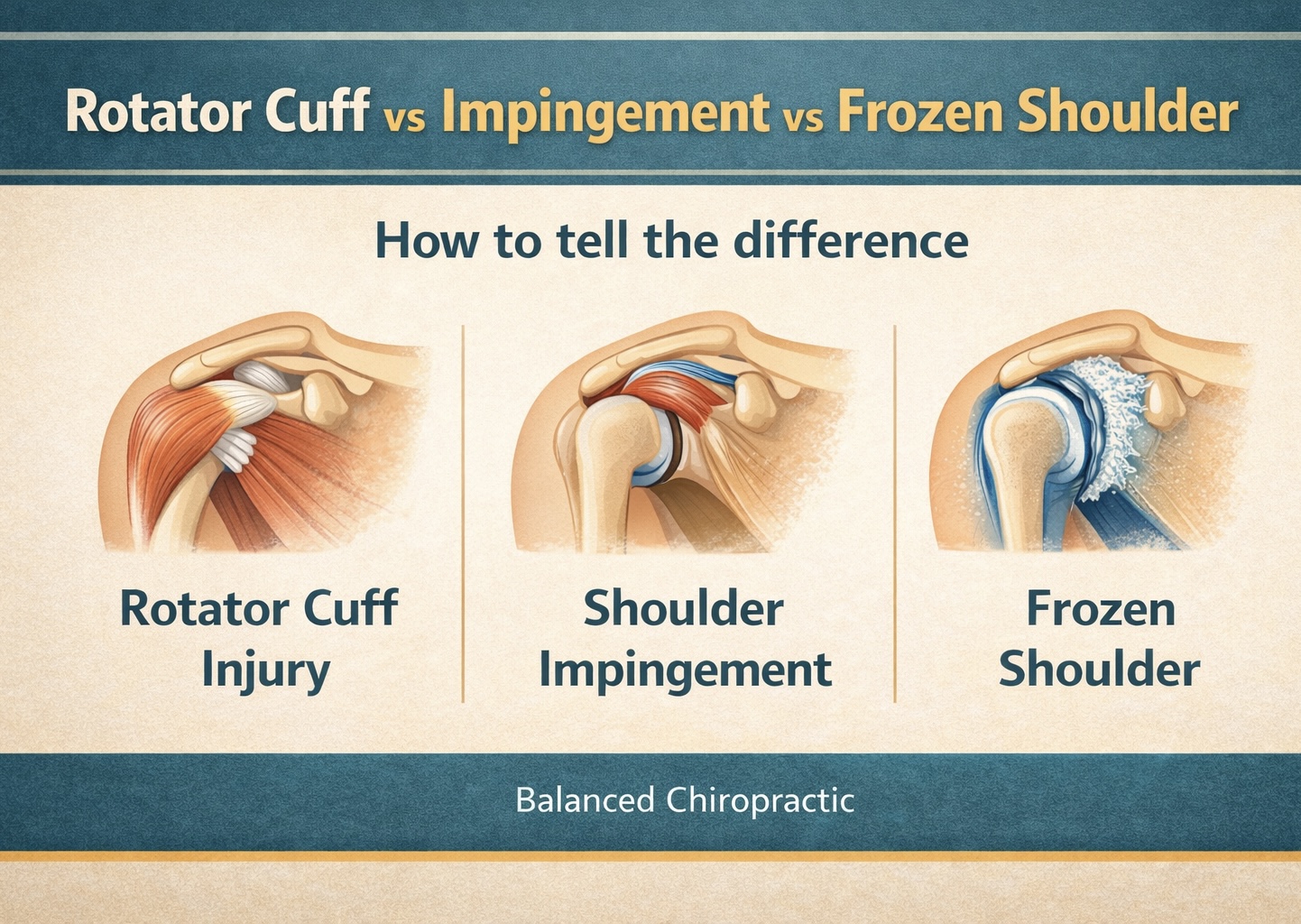
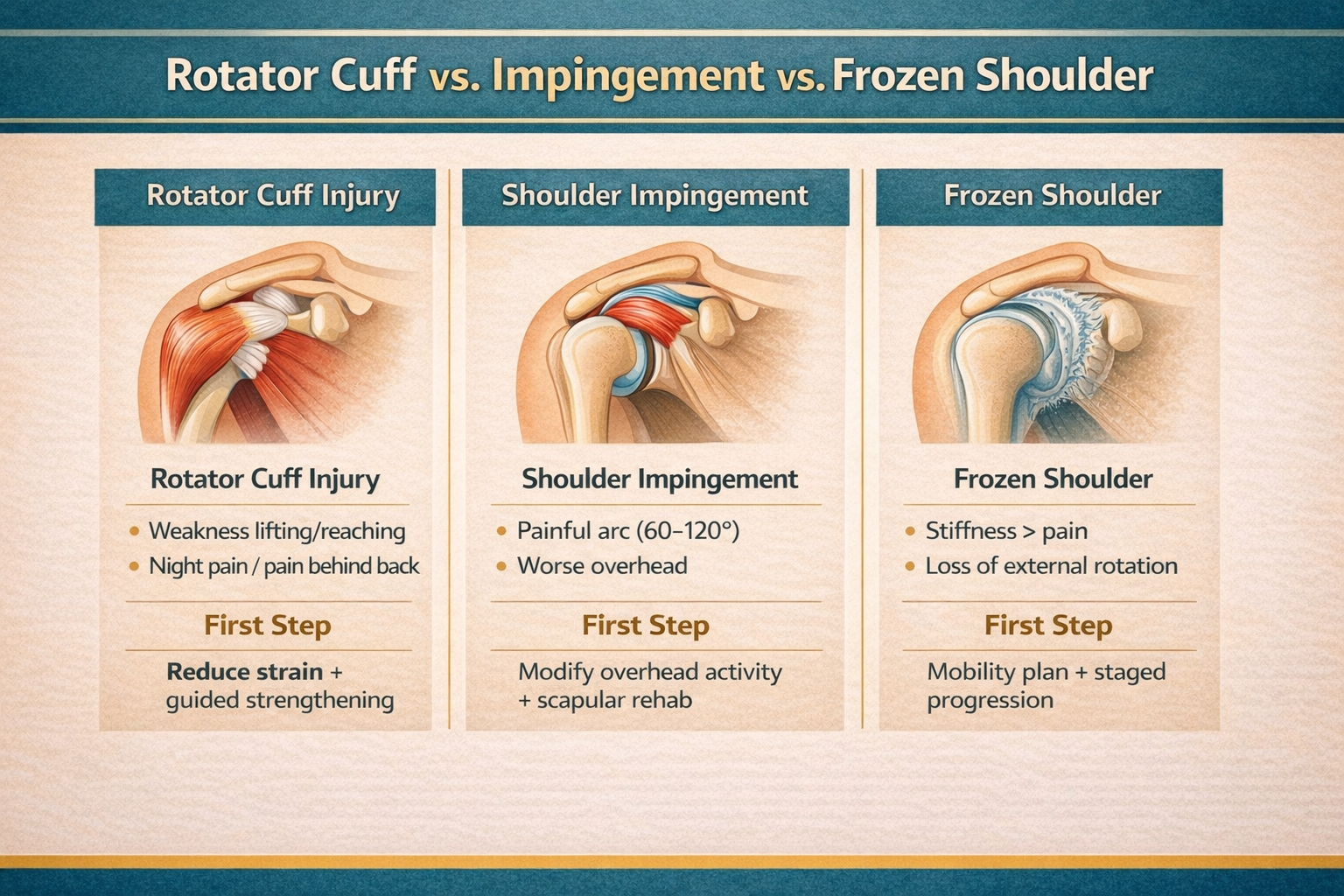
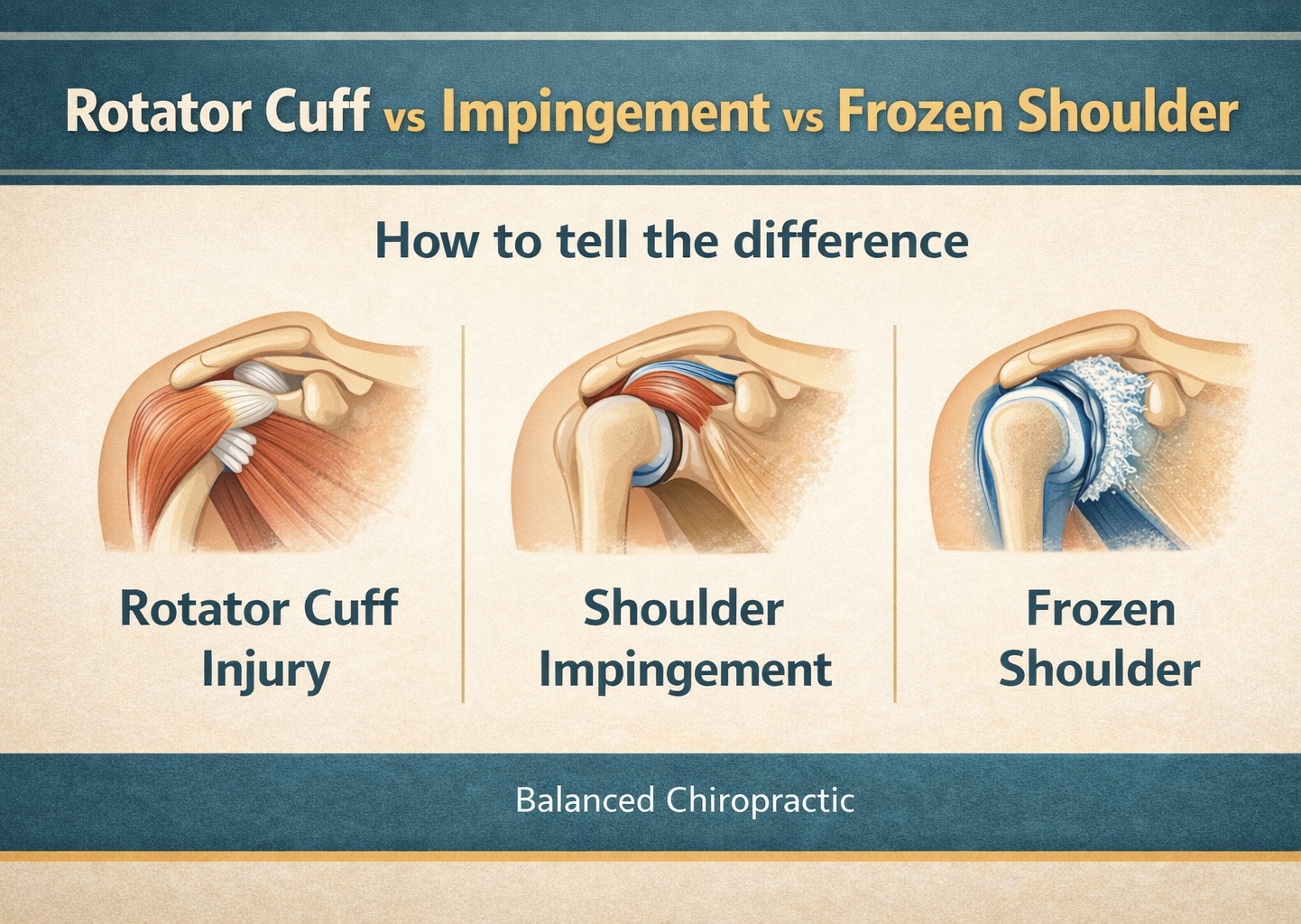
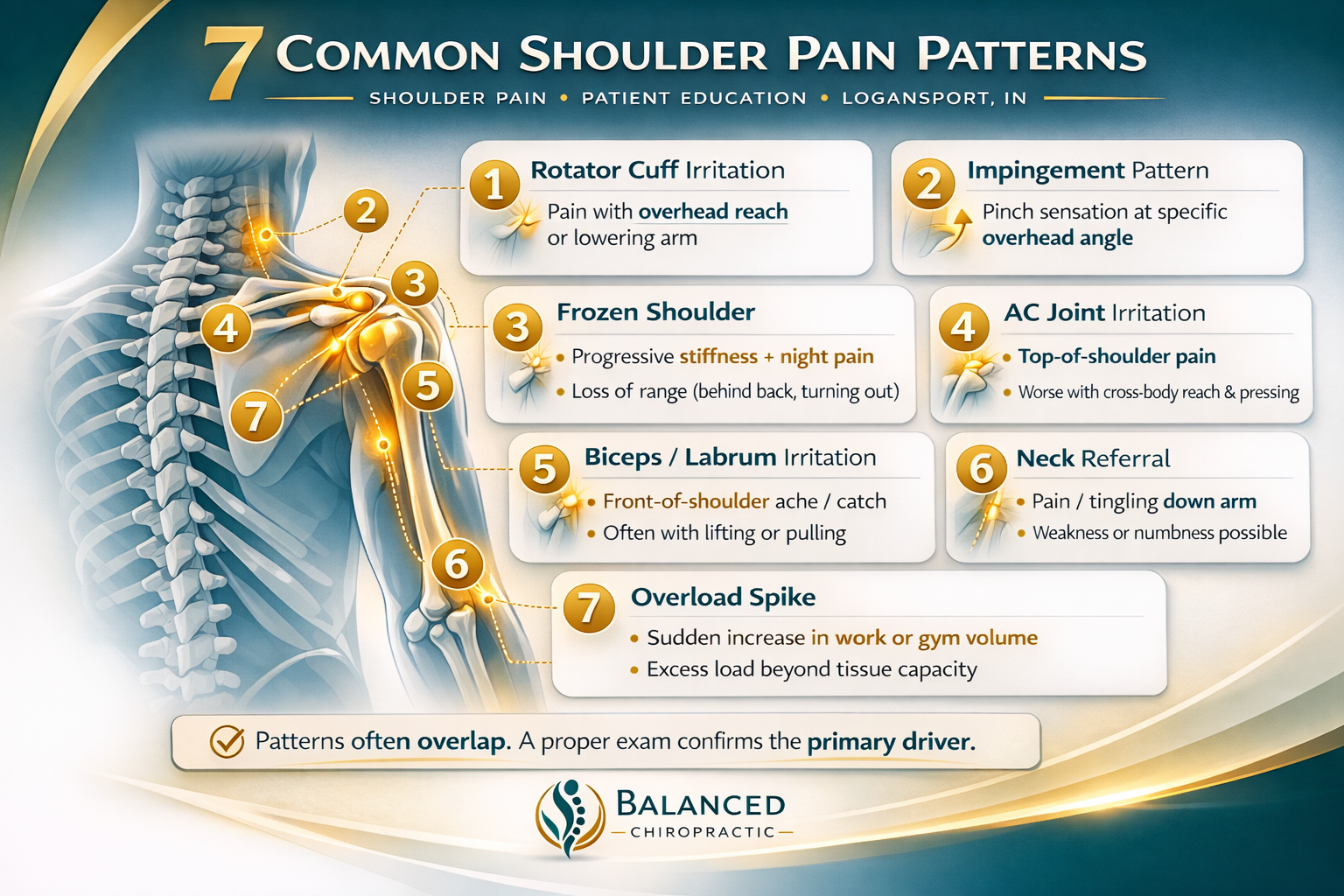
Why It Happens (Top Patterns)
Use pain location + stair clues to narrow the most likely driver.
Patellofemoral pain (kneecap overload)
Feels like: front-of-knee ache, worse downstairs or after sitting.
Helps first: reduce spike + quad/hip progression + technique.
Patellar tendon irritation
Feels like: pain just below kneecap, worse with jumping/squats/stairs.
Helps first: isometrics + graded loading (not total rest).
Meniscus irritation pattern
Feels like: inside joint-line pain, catching, swelling after activity.
Helps first: evaluation + smart load plan; avoid twisting under load.
Arthritis / joint irritation
Feels like: stiffness + ache, often worse after inactivity.
Helps first: low-impact movement + strength + tolerance building.
Hip weakness / valgus control (knee collapses inward)
Feels like: front/inside pain with stairs or step-downs.
Helps first: glute control + single-leg stability progression.
Lateral/IT band–type pattern (less common)
Feels like: outside knee pain, often with repetitive steps.
Helps first: hip control + volume management + mechanics.
Not sure which one fits?
If you’re deciding between runner’s knee vs meniscus, start here: Runner’s Knee vs. Meniscus (How to Tell).
5 Fixes That Usually Help (Mini Protocols)
Use the next-day rule: you should feel the same or better the next day (mild soreness is okay).
Fix #1: Reduce the spike (7–14 days)
- Use the rail temporarily, slow down, and reduce total stair reps
- Choose shorter steps when possible
- Avoid deep loaded knee bends that spike pain
Fix #2: Quad capacity (the biggest win)
- Start with pain-safe quad isometrics (short holds)
- Progress to step-downs or sit-to-stands in a tolerable range
- Progress volume before intensity
Fix #3: Hip/glute control
- Band walks or side-steps (tolerable dose)
- Single-leg balance work with good alignment
- Reduce knee “collapse” during stairs/step-downs
Fix #4: Mobility that actually helps
- Ankle mobility (if you feel forced into awkward knee angles)
- Hip mobility (pain-safe)
- Avoid aggressive knee stretching into sharp pain
Fix #5: Technique tweaks (stairs & squats)
- Downstairs: slow the lowering (eccentric control)
- Use the whole foot (“tripod”), not just toes
- Small forward trunk lean can reduce kneecap load for some people
If you suspect arthritis patterns
A low-impact movement plan can help: A 7-Day Low-Impact Movement Plan for Arthritis.
Up vs Down Stairs (Why Down Usually Hurts More)
Downstairs demands more braking (eccentric control). That’s why kneecap/tendon patterns show up fast.
Downstairs tips (high ROI)
- Use the rail short-term while you rebuild strength
- Slow down (control the descent)
- Reduce step height or number of trips temporarily
- Stop if form collapses or pain spikes sharply
Simple rule
If downstairs is the main trigger, quad endurance + step-down progression is usually the best long-term fix.
When to Worry (Red Flags)
Get checked promptly if any of these are present.
- True locking (knee gets stuck)
- Repeated giving way or sudden instability
- Large swelling or rapidly worsening swelling
- Unable to bear weight or severe worsening pain
- Fever/hot red joint or feeling very unwell
- Major trauma (fall, collision)
- Severe night pain that keeps escalating
If you’re unsure, start with Contact & Location and we’ll guide you.
Knee Pain on Stairs FAQs
Quick answers—including meniscus questions and imaging.